Many rehabilitation interventions have been recommended for patients with rheumatic disease. This section presents an overview of indications and contraindications of the most common rehabilitation interventions used in patients with rheumatic disease.
Education and self-management
Education and self-management are widely regarded as being fundamental to the comprehensive management of rheumatic diseases, in particular rheumatoid arthritis. Patient associations in North America have been instrumental in developing and making available multiple resources. Self-management training can be provided by other patients or by healthcare providers. The programs provided by peers have been extensively
studied and shown to improve pain, function, selfefficacy, and satisfaction.86 They can reduce visits to healthcare providers and associated costs. Programs provided by care providers have been less studied but appear to provide similar benefits.
The programs with the best results focus on active learning in peer groups, with an emphasis on problem solving and increasing self-efficacy. They also include information on the nature and prognosis of arthritis; efficacy and side effects of arthritis medications; and exercise, pacing, and other rehabilitation interventions.
Exercise, rest, and energy conservation
Exercise and exercise-based rehabilitation programs are interventions well supported in controlled trials. Exercise improves range of motion, strength, and functional activities in osteoarthritis, rheumatoid arthritis, and extraarticular rheumatism.
The exercise program must be individualized according to the disease activity, accumulated joint damage,
and the patient's goals and interests.
In general terms, high-impact exercises such as jumping, basketball, etc. should be avoided in patients
with significant rheumatic disease. Medium-impact exercises such as walking, jogging, bicycling, and swimming are appropriate, unless there is severe joint inflammation.
Severely inflamed joints should only be subjected to gentle mobilization and stretching within the available range of movement.
Strategies for joint protection, energy conservation, and pacing are frequently recommended by occupational therapists. Often, patients develop their own strategies for energy conservation. However, there is limited evidence of efficacy in this regard.
Physical modalities
Heat, cold, and other physical modalities have been used to treat rheumatic conditions for centuries.Most of these modalities have been accepted by tradition, and only recently have been subjected to controlled trials,also Local heat can decrease pain, at least temporarily, and can be easily applied by patients or family members if precautions to avoid burns are taken.There is a theoretic possibility that local heat can
increase the inflammatory response and possibly increase joint damage, but this has not been supported empirically.The usual contraindications to local heat application. Local heat can be applied by conduction (heat pads and water bottles), radiation (incandescent lamps and infrared lamps), or immersion (hot water, paraffin baths, and mud baths) .There is no solid evidence that one method is preferable to another, and the choice depends on availability and the body part to be treated. For example, paraffin baths are ideally
suited to apply heat to the rheumatic hand.Cold and contrast baths (heat alternating with cold) have been described, but there are no adequate studies to support their utility in rheumatic disease. In the absence of conclusive scientific evidence, the patient's comfort and preferences should take precedence.
Ultrasound and diathermy mostly function as conversion methods of applying heat to the deeper tissues, although there might be additional mechanisms at play.Recent studies have reported the use of shock waves to treat tendonitis and fasciitis, but rigorous randomized trials have questioned their efficacy.
Interferential currents have little application for treating joint disease, but functional electrical stimulation is sometimes used to prevent muscle atrophy during episodes of intense disease activity.
Transcutaneous electrical nerve stimulation might relieve the pain of rheumatic disease,and
animal studies suggest it can also decrease joint swelling.
Electromagnetic fields have established efficacy in accelerating fracture healing,' and available trials suggest some benefit in knee osteoarthritis. Low-power laser has been poorly studied but might provide short-term relief of pain and stiffness.
Manual and mechanical therapies
Manual therapies have been extensively used to treat regional musculoskeletal pain and extraarticular rheumatism.They are seldom prescribed in rheumatoid arthritis or severe osteoarthritis, because they are typically considered to be alternative or integrative therapies. Nevertheless, many patients make use of them outside the medical establishment.
Traction is sometimes recommended for patients with back or neck pain, but randomized controlled trials have not demonstrated benefit.
Acupuncture could be classified as a mechanical therapy, in that it produces mechanical stimulation by the needle, but diverse theories exist about its mechanism of action.Controlled studies are rare, but preliminary evidence suggests benefits in osteoarthritis of the knee.
Subscribe to:
Post Comments (Atom)


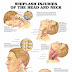


Fibromyalgia is difficult to diagnose, diagnosis is based on the history and the examination of the patient by a doctor. Blood tests are usually made to eliminate other causes for the symptoms of patients. According to the criterion of American College of Rheumatology, a person has Fibromyalgia if he or she have extended at least three months and acute pain, then pain is at least from 11 to 18 in the hypersensitive points in the body.
ReplyDeleteAgustin Legido
Findrxonline
Thank you for your notice Agustin :)
ReplyDelete